HOME➢fructose testing in male infertility
fructose testing in male infertility
Goal to help childless couples enjoy the Joy of Parenting
Call For a Free Quote
(+91) 97910 85541
Or Send a Message
Fructose Testing in Male Infertility
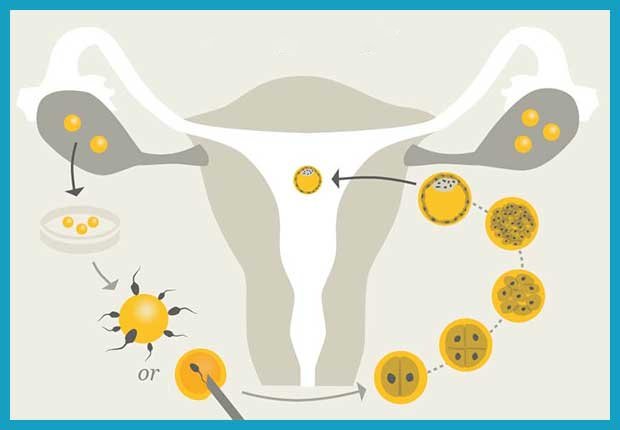
Fructose testing, also known as the semen fructose test, is a key laboratory procedure used in the evaluation of male infertility. This test measures the concentration of fructose—a sugar produced by the seminal vesicles—in a semen sample. Fructose serves as a crucial energy source for sperm, supporting their motility and fertilizing ability.
What Does Fructose Testing Assess?
- Seminal Vesicle Function:Normal fructose levels indicate that the seminal vesicles are functioning properly and contributing their secretions to semen.
- Obstructive Disorders:Low or absent fructose suggests blockages in the reproductive tract (such as ejaculatory duct obstruction), congenital absence or dysfunction of the seminal vesicles, or, less commonly, hormonal imbalances.
- Azoospermia Evaluation:In cases of azoospermia (no sperm in semen), fructose testing helps distinguish between obstructive (blockage) and non-obstructive (testicular failure) causes.
How is the Test Performed?
- Sample Collection:A semen sample is collected, usually after 2–7 days of abstinence, in a sterile container.
- Laboratory Analysis:The sample is analyzed for fructose concentration. No fasting is required for this test.
- Interpretation:
- Normal fructose:Indicates healthy seminal vesicle function.
- Low/Absent fructose:Suggests obstruction or seminal vesicle dysfunction, prompting further investigation with imaging, hormone tests, or genetic studies.
Clinical Importance
- Diagnosis of Male Infertility:The test is a vital part of comprehensive semen analysis, helping to uncover causes of infertility such as ejaculatory duct obstruction or seminal vesicle issues.
- Treatment Guidance:Results guide further diagnostic steps and treatment, such as surgical correction of blockages or medical management of underlying conditions.
- Monitoring:Useful for assessing the success of treatments like surgery for duct obstruction.
Key Points
- Fructose is essential for sperm motility and energy.
- Low or absent fructose in semen is a marker of possible reproductive tract obstruction or seminal vesicle dysfunction.
- The test is simple, non-invasive, and provides valuable information for diagnosing and managing male infertility.
Recurrent Pregnancy Loss (RPL)
Recurrent pregnancy loss is defined as two or more consecutive miscarriages (spontaneous abortions) before 20 weeks of gestation. It affects about 1–2% of women, and each loss can be physically and emotionally challenging.
Causes of Recurrent Pregnancy Loss
RPL has multiple potential causes, which can be classified as maternal, paternal, fetal, or placental:
Maternal Causes
- Uterine or cervical abnormalities:Polyps, fibroids (myomas), adhesions, or cervical insufficiency.
- Endocrine disorders:Poorly controlled thyroid disease (hypo- or hyperthyroidism), diabetes mellitus, polycystic ovary syndrome (PCOS), luteal phase defect, and hyperprolactinemia.
- Acquired thrombotic disorders:Especially antiphospholipid syndrome (APS), which is associated with recurrent losses after 10 weeks.
- Chronic medical conditions:Hypertension, chronic kidney disease, systemic lupus erythematosus (SLE).
Paternal Causes
- Chromosomal abnormalities:Such as balanced translocations.
- Semen quality:Certain abnormalities in semen analysis may increase miscarriage risk.
Fetal Causes
- Chromosomal or genetic abnormalities:These are the most common cause, accounting for up to 50% of miscarriages. Aneuploidy (abnormal number of chromosomes) is involved in up to 80% of losses before 10 weeks.
- Anatomic malformations.
Placental Causes
- Placental insufficiency or abnormalitiesdue to chronic maternal disease.
Diagnostic Evaluation
A thorough evaluation is recommended after two or more losses, especially if the woman is over 35, has had difficulty conceiving, or if fetal cardiac activity was previously detected. The workup may include:
- Parental karyotyping(chromosome analysis)
- Uterine imaging:Hysterosalpingography, ultrasound, or hysteroscopy to assess for anatomical abnormalities
- Thyroid function testsand assessment for other endocrine disorders
- Screening for antiphospholipid antibody syndrome (APS)
- Selected thrombophilia testingif indicated
Treatment and Prognosis
- Treatable causes(e.g., uterine abnormalities, endocrine disorders, APS) should be addressed with surgery, medications, or anticoagulation as appropriate.
- Genetic counselingand assisted reproductive technologies (such as IVF with preimplantation genetic testing) may be considered for chromosomal causes.
- Progesterone supplementationmay help reduce miscarriage rates in women with unexplained RPL.
- Psychological support and counselingare important for all couples experiencing RPL.
Even after several losses, the prognosis remains good: more than 60–65% of women with RPL will have a successful live birth in subsequent pregnancies, depending on the underlying cause and number of prior losses.
Multiple Abortion (Repeated Pregnancy Loss / Recurrent Miscarriage)
Multiple abortion, medically referred to as recurrent pregnancy loss (RPL) or repeated miscarriage, is defined as two or more consecutive pregnancy losses before 20 weeks of gestation. This condition affects up to 1–2% of couples trying to conceive and can have significant physical and emotional impacts.
Causes
Multiple abortions can result from a variety of factors:
- Genetic abnormalities:Chromosomal issues in the embryo are the most common cause, especially in early miscarriages. Parental chromosomal rearrangements (such as balanced translocations) are found in about 4–5% of couples with RPL.
- Uterine abnormalities:Congenital (septate or double uterus) or acquired (fibroids, polyps, adhesions) uterine issues can account for up to 15% of cases.
- Endocrine disorders:Poorly controlled thyroid disease, diabetes, polycystic ovary syndrome (PCOS), and high prolactin can increase miscarriage risk.
- Immunological factors:Conditions like antiphospholipid syndrome (APS) or other clotting disorders are linked to recurrent losses, especially after 10 weeks.
- Chronic medical conditions:Hypertension, chronic kidney disease, and autoimmune diseases (e.g., lupus) can contribute.
- Lifestyle factors:Smoking, alcohol, drug use, obesity, and excessive caffeine intake may increase miscarriage risk and should be addressed.
- Male factors:Abnormal semen parameters and advanced paternal age may play a role, though evidence is less clear.
Diagnosis
A thorough evaluation is recommended after two or more losses and includes:
- Detailed medical history and physical examination
- Blood tests for hormonal imbalances, clotting disorders, and autoimmune markers
- Genetic testing (karyotyping) of both partners
- Imaging studies (ultrasound, hysteroscopy) to assess uterine structure
Treatment
Treatment is tailored to the underlying cause, if identified:
- Genetic counseling:For couples with chromosomal rearrangements; IVF with preimplantation genetic testing (PGT-SR) may be considered.
- Surgery:To correct uterine abnormalities (e.g., septum, fibroids, polyps) via hysteroscopic procedures.
- Hormonal therapy:To manage thyroid, prolactin, or other endocrine issues.
- Blood-thinning medications:Low-dose aspirin and heparin for women with antiphospholipid syndrome or certain clotting disorders.
- Lifestyle modifications:Smoking cessation, reducing alcohol/caffeine, weight management, and stress reduction.
- Emotional support:Psychological counseling and support groups are vital due to the emotional toll of repeated losses.
For about 40–50% of couples, no clear cause is found. Even in these cases, the prognosis is often good—almost two-thirds of women with RPL will eventually have a healthy pregnancy, sometimes without additional treatment.
High Risk Pregnancy
A high-risk pregnancy is one in which the mother, fetus, or both have an increased chance of health problems or complications before, during, or after delivery. This designation is based on the presence of certain risk factors that can threaten the health or life of the mother or baby and often requires specialized care and closer monitoring throughout pregnancy.
Common Risk Factors for High-Risk Pregnancy
- Maternal age:Younger than 17 or older than 35 years
- Pre-existing medical conditions:Such as high blood pressure, diabetes, kidney disease, heart disease, epilepsy, thyroid disorders, autoimmune diseases (e.g., lupus), or HIV
- Obstetric history:Previous preterm birth, previous C-section, recurrent miscarriages, or having a child with a genetic disorder or birth defect
- Lifestyle factors:Smoking, alcohol use, drug use, being significantly underweight or overweight
- Pregnancy-related conditions:Multiple gestation (twins, triplets), gestational diabetes, preeclampsia, placenta previa, or abnormal uterine structure
- Genetic or structural fetal abnormalities
- Infections:Sexually transmitted diseases, urinary tract infections, or other significant infections during pregnancy
Management and Care
- Early and regular prenatal careis essential for high-risk pregnancies to monitor for complications and optimize outcomes.
- Specialized care:High-risk pregnancies often require a multidisciplinary team, including maternal-fetal medicine specialists.
- Lifestyle modifications:Maintaining a healthy diet, managing weight, avoiding harmful substances, and controlling chronic conditions.
- Close monitoring:More frequent prenatal visits, ultrasounds, blood tests, and sometimes referral to a perinatal center for advanced care.
- Preconception counseling:For women with known risk factors, pre-pregnancy evaluation and management can help reduce risks.
Prognosis
While a high-risk pregnancy increases the likelihood of complications, many women with high-risk pregnancies go on to have healthy babies with appropriate medical care and monitoring. The key is early identification of risk factors and individualized management throughout the pregnancy.
Obstetric Doppler
Obstetric Doppler ultrasound is a specialized imaging technique used during pregnancy to assess blood flow in the placenta, umbilical cord, and fetal vessels. It plays a crucial role in monitoring fetal well-being, especially in high-risk pregnancies, by providing real-time information about the circulation between mother and baby.
Key Uses and Benefits
- Assessment of Blood Flow:Doppler ultrasound evaluates blood flow in the uterine arteries, umbilical artery, and fetal vessels, ensuring the fetus is receiving adequate oxygen and nutrients for healthy growth.
- Detection of Complications:It helps identify placental insufficiency, umbilical cord abnormalities, and fetal vascular problems, which can lead to growth restriction, preeclampsia, or fetal distress if not detected early.
- Guiding Prenatal Care:Results from Doppler studies inform decisions about the timing and type of interventions, such as adjusting treatment plans or determining the optimal time for delivery in high-risk pregnancies.
- Monitoring High-Risk Pregnancies:Regular Doppler assessments are especially important for pregnancies complicated by hypertension, diabetes, multiple gestations, or previous pregnancy complications.
Clinical Impact
- Improved Outcomes:Use of Doppler ultrasound in high-risk pregnancies is associated with a reduction in perinatal deaths, fewer inductions of labor, and fewer hospital admissions, without an increase in adverse effects.
- Non-Invasive and Safe:The procedure is painless, does not use ionizing radiation, and can be repeated as needed throughout pregnancy.
How It Works
A Doppler transducer is placed on the mother’s abdomen. It emits sound waves that bounce off moving blood cells, allowing visualization and measurement of blood flow patterns in maternal and fetal vessels. Color Doppler enhances this by providing real-time images of circulation.
When Is It Used?
- Routinely in high-risk pregnancies or when fetal well-being is in question
- When there is concern about fetal growth, maternal hypertension, diabetes, or suspected placental or cord abnormalities
NT Scan (Nuchal Translucency Scan)
An NT scan (Nuchal Translucency scan) is a specialized ultrasound performed in the first trimester, typically between 11 and 14 weeks of pregnancy. It measures the thickness of the fluid-filled space at the back of the fetus’s neck, known as the nuchal translucency.
Purpose
- Screening for Chromosomal Abnormalities:The NT scan is a key part of early prenatal screening for genetic conditions such as Down syndrome (trisomy 21), Edwards syndrome (trisomy 18), and Patau syndrome (trisomy 13).
- Detection of Heart Defects:An increased NT measurement may also indicate a higher risk of congenital heart defects or other structural anomalies.
- Combined Screening:The NT scan is often combined with a maternal blood test to improve accuracy in estimating the risk of chromosomal abnormalities.
How the NT Scan is Performed
- Preparation:Usually performed transabdominally, but may be done transvaginally for clearer images.
- Ultrasound Procedure:A gel is applied to the abdomen, and the ultrasound probe is used to visualize the fetus.
- Measurement:The sonographer measures the thickness of the nuchal translucency, which appears as a dark space at the back of the baby’s neck.
- Timing:The scan is most accurate between 11 weeks + 3 days and 13 weeks + 6 days of gestation.
Interpretation of Results
- Normal Range:NT measurements typically range from 1.3 to 2.7 mm. An NT measurement of 5 mm or more is considered increased and may indicate a higher risk for chromosomal or structural abnormalities.
- Screening, Not Diagnosis:The NT scan is a screening test, not a diagnostic test. A higher measurement suggests increased risk but does not confirm a diagnosis.
- Next Steps:If the NT measurement is increased, further diagnostic tests such as Non-Invasive Prenatal Testing (NIPT), chorionic villus sampling (CVS), or amniocentesis may be recommended.
Additional Information
- Optional Test:The NT scan is optional and should be discussed with your healthcare provider.
- Other Uses:The scan can also help confirm gestational age, detect multiple pregnancies (twins, etc.), and assess basic fetal anatomy.
Anomaly Scan (Anatomy Scan / 20-Week Ultrasound)
An anomaly scan—also called the anatomy scan or 20-week ultrasound—is a detailed prenatal ultrasound performed between 18 and 22 weeks of pregnancy. Its primary purpose is to systematically examine the fetal anatomy, detect structural abnormalities, and assess fetal growth, placental position, and amniotic fluid volume.
What Does the Anomaly Scan Check?
The scan evaluates the following fetal structures and organs in detail:
- Brain and Spine:Detects neural tube defects and brain malformations.
- Face:Checks for cleft lip, palate, and other facial anomalies.
- Heart:Assesses heart chambers and vessels for congenital heart defects.
- Abdomen:Examines the stomach, kidneys, bladder, and bowel for anomalies.
- Limbs:Ensures proper development of arms, legs, hands, and feet.
- Placenta and Amniotic Fluid:Evaluates placental position (e.g., placenta previa), structure, and amniotic fluid volume.
- Maternal Pelvic Organs:Assesses uterus, cervix, and ovaries for abnormalities.
Conditions Identified
The anomaly scan can detect a wide range of fetal, placental, and maternal conditions, including:
|
Fetal Conditions |
Placental Conditions |
Maternal Conditions |
|
Anencephaly, spina bifida, |
Placenta previa, |
Uterine anomalies, fibroids, |
|
cleft lip, congenital heart |
vasa previa, |
short cervix |
|
defect, diaphragmatic hernia, |
placenta accreta, |
|
|
omphalocele, renal agenesis, |
velamentous cord |
|
|
skeletal dysplasias, |
insertion |
|
|
Edwards/Patau syndromes |
Importance
- Early Detection:Identifies major structural abnormalities and congenital malformations, some of which may require intervention after birth or influence delivery planning.
- Growth Monitoring:Measures fetal size to monitor growth patterns and detect growth restriction.
- Placental Assessment:Helps plan delivery if placental problems (e.g., placenta previa) are detected.
- Pregnancy Management:Guides further testing, counseling, and management if abnormalities are found.
Limitations
- Not All Anomalies Detected:Sensitivity varies; some conditions may be missed due to fetal position, maternal obesity, or the nature of the anomaly.
- Cannot Detect Functional or Genetic Disorders:Conditions like cerebral palsy or autism cannot be diagnosed by this scan.
- Sex Determination:Fetal sex can often be seen, but sex determination for non-medical reasons is prohibited in many countries, including India.
Safety
- Non-invasive and Safe:Uses sound waves, not radiation, and is considered safe for both mother and fetus.
Why Choose Us?
Are you ready to embark on the journey of a lifetime? At Jeevan Mithra Fertility Centre, we’re here to guide, helping you realize your dream of becoming a parent.
Experience Professional
state of the art facilities
personalized care

Email Us
OFfice
opp to Koyambedu Bus Stand, Chennai-600 106
